How was pressotherapy developed?
Pressotherapy was developed with the intent to treat mainly circulatory disorders with a:
- lymphatic origin
- venous origin
- mixed origin
In aesthetic treatments, it can also be used for:
- lymphatic drainage massage of the legs and arms
- water retention
- cellulite
- swollen or heavy feet and legs
- relaxation and cramp prevention
- overweight
- toning
The fundamental factor on which pressotherapy acts is oedema.
What is the pathophysiological mechanism that pressotherapy acts against?
1 the flow of blood is slowed down or hindered (due to alteration of the valvular system or insufficiency of the skeletal-muscle pump)
2 increases perivascular oncotic and osmotic pressure
3 increased interstitial pressure.
The result: water retention and oedema leading to a lower supply of oxygen and nutrients to the cells, which will consequently work less and badly.
In case of vascular disorders this stasis is mainly localised at the suprapatellar and perimalleolar level.
How does pressotherapy work?
With this method, a gradual pressure is exerted on the affected tissues in order to generate a distal-proximal pressure gradient. This is alternated with release phases. The sequencing and intermittence of the compression combined with the uniform application, peristalsis and gradual pressure lead to an increase in centripetal hemolymphatic drainage, as they generate:
- Increased venous flow velocity in the compressed area (due to the reduction in vessel size) with vessel relaxation in the downstream area
- Increase in lymphatic flow velocity and initial flow rate (for fluid resorption)
This, in addition to visibly reducing oedema , also brings about a physiological response of the endothelial cells by releasing substances with antithrombotic, profibrinolytic and vasodilator activity.
Of course it is not possible to eliminate the obstruction, and therefore the cause upstream, but it proves to be very effective in the water component of initial lymphoedema.
Pneumatic pressotherapy can be added to manual lymphatic drainage, bandaging, gymnastic decongestion, biostimulation and skin care. All this must take place under medical supervision as in some cases it is necessary to avoid a fibrosclerotic evolution owing to the rapid osmotic restoration of the water component immediately after the pressure due to the loss of fluids.
What factors should be evaluated in order to set up an adequate treatment and which influence the result?
- The type of equipment used
- The compression sequence
- The pressure applied and the duration it is applied
- The clinical stage of the disease
- The patient's tolerability
It is important to bear in mind that higher pressures do not always correspond to greater effects and benefits; the maximum pressure exerted with pressotherapy should not exceed the minimum blood pressure, so as not to hinder the arrival of oxygenated blood in the tissues and thus avoid the risk of muscle ischaemia. It is therefore essential to assess on a case-by-case basis and perform a Doppler ultrasound exam in cases of lymphoedema with fibrosclerosis, in order to establish up to which pressure parameters can be reached.
Treatment
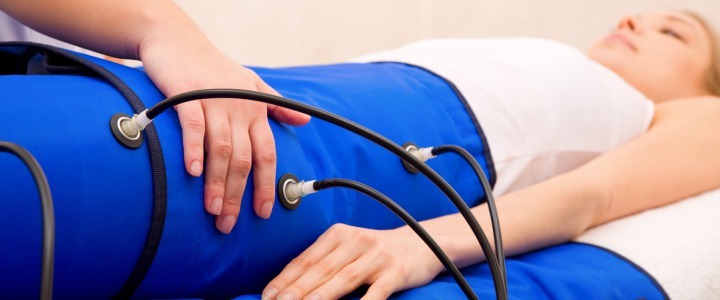
The inflatable air cushions are placed on the areas to be treated, then several chambers inflate sequentially across the various sections (the legs, the arms and abdominal/gluteal bands) creating a wave of pressure. The greater number of inflatable elements allows for a better fragmentation of the oedema, obtaining a greater and more homogeneous capacity for fluid drainage.
At the end of the treatment, increased diuresis is normal as drainage is increased while another part of the mobilised fluids is recovered from capillary microcirculation. In this way we will also achieve a detoxifying effect of the whole organism as well as the disposal of toxins.
To achieve a clear reduction in volume, several treatments must be carried out.
Contraindications
Pressotherapy treatment is contraindicated in people with heart failure as the cardiac preload associated with water resorption may increase rapidly, as well as in patients with uncontrolled hypertension. In patients with arteriopathy, the pressure applied to the skin microcirculation may induce the appearance of ischaemic skin lesions.
It is also absolutely contraindicated in patients with recent venous thrombosis because the risk of pulmonary embolism is increased.
In patients with skin infections, the increase in lymphatic output may promote microbial dissemination.
Also not recommended during pregnancy or cancer treatments.



(maximum 1000 characters)
Comment on the article